Hyperkalemia in CKD: Potassium Diet Limits and Emergency Care
Imagine waking up with a strange feeling of muscle weakness or a fluttering in your chest, only to find out your blood chemistry is in a dangerous zone. For people living with hyperkalemia in CKD is a condition where serum potassium levels rise above 5.0 mmol/L due to the kidneys' inability to filter excess potassium from the blood. While potassium is essential for your heart to beat and muscles to move, too much of it acts like a poison to the electrical system of your heart. In advanced stages of kidney disease, nearly half of all patients struggle with this imbalance, creating a high-stakes tug-of-war between protecting the heart and keeping potassium levels safe.
The RAASi Dilemma: Why Potassium Spikes
Most people with kidney disease are prescribed RAASi (Renin-Angiotensin-Aldosterone System inhibitors). These drugs are lifesavers-they protect the heart and slow down the progression of kidney failure. However, they come with a catch: they tell your body to hold onto potassium. This creates a clinical paradox where the very medicine keeping your kidneys functioning can push your potassium levels into the danger zone.
If you're on these medications, you might feel fine until your levels hit a critical point. That's why monitoring is non-negotiable. According to KDIGO guidelines, you should have your potassium checked within two weeks of starting these meds, and then every few months once you're stable. Waiting for symptoms is a gamble you can't afford to take.
Setting Your Potassium Budget: Diet Limits by Stage
Managing your diet isn't about banning potassium entirely-it's about a "potassium budget." Depending on how well your kidneys are working, your daily limit changes. If you are in the early stages (CKD 1-3a), you generally don't need restrictive limits; a "prudent" approach to eating is usually enough. However, once you hit advanced stages (3b-5), the rules get strict.
For those in advanced CKD not yet on dialysis, the gold standard is to limit potassium intake to between 2,000 and 3,000 mg per day. To put that in perspective, a single medium banana has about 422 mg of potassium per 100g. If you eat a few of those along with a potato, you've already used up a huge chunk of your daily budget.
| Food Item | Potassium Amount (mg) | Impact Level |
|---|---|---|
| Bananas | 422 mg | High |
| Potatoes | 421 mg | High |
| Oranges | 181 mg | Moderate |
| Apples | 107 mg | Low |
Pro tip: Don't just rely on memory. Use smartphone apps that scan barcodes to track your real-time intake. Many patients find that the "social isolation" of a strict diet is the hardest part, so focusing on low-potassium swaps-like berries instead of bananas-can make the lifestyle more sustainable.

Emergency Treatment: When it Becomes a Crisis
When potassium levels climb to 5.5 mmol/L or higher, it's no longer about diet; it's about medical intervention. If levels hit 6.0 mmol/L or you see "peaked T-waves" on an ECG, you are in an emergency. Doctors use a three-pronged attack to stabilize you and get the potassium out of your system.
- Stabilizing the Heart: Calcium Gluconate is given via IV. It doesn't actually lower potassium, but it acts like a shield for your heart membrane, preventing lethal arrhythmias for about 30 to 60 minutes.
- Shifting Potassium: An insulin-glucose protocol (10 units of insulin with 50% dextrose) is used to push potassium from the blood back into the cells. This works quickly-usually within 15 to 30 minutes-but carries a risk of crashing your blood sugar.
- Flushing the System: If you have metabolic acidosis, sodium bicarbonate may be used to help shift potassium levels.
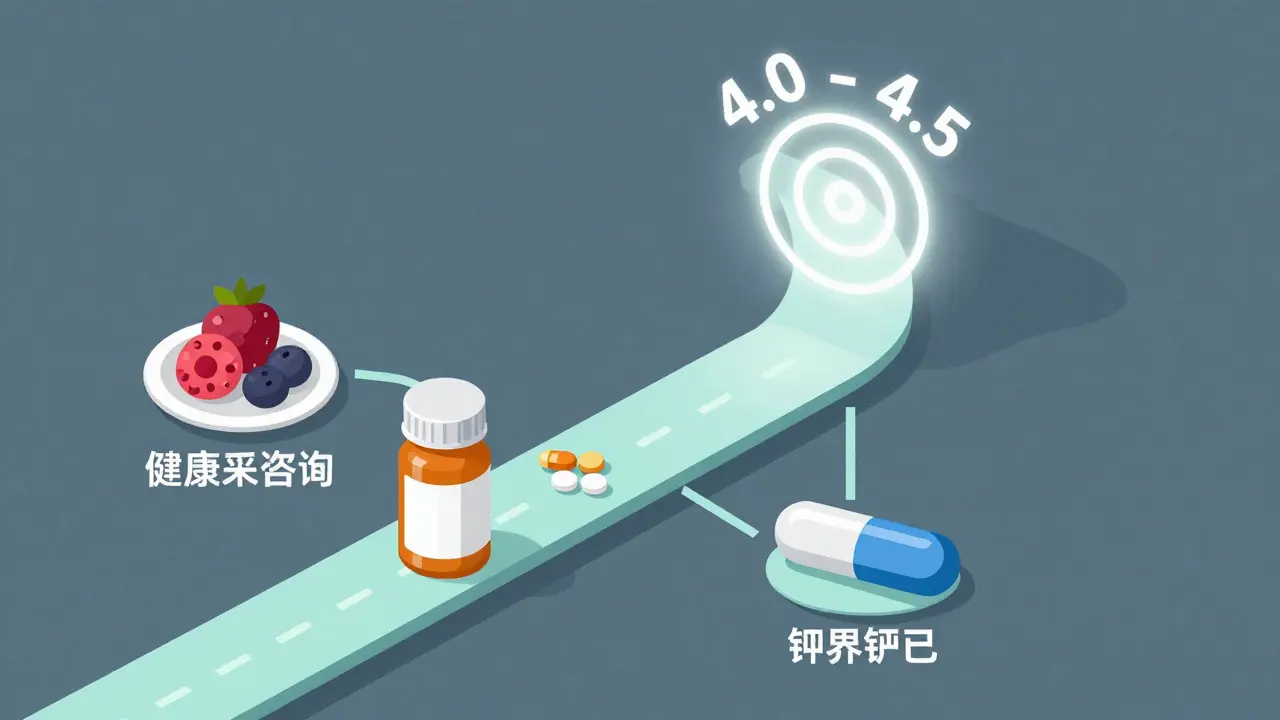
Modern Solutions: The New Wave of Potassium Binders
For a long time, doctors relied on Sodium Polystyrene Sulfonate (SPS. While cheap, it's far from ideal. It's slow and carries a rare but terrifying risk of colonic necrosis. Thankfully, newer medications have changed the game, allowing more patients to stay on their heart-protecting RAASi meds without fear.
Today, we have two main modern alternatives: Patiromer and Sodium Zirconium Cyclosilicate (SZC). SZC is the "sprinter"-it can drop potassium levels significantly within a single hour, making it great for acute spikes. Patiromer is more of a "marathon runner," better suited for long-term maintenance because it doesn't add as much sodium to your system, which is crucial for people with heart failure who struggle with edema.
| Attribute | SPS (Traditional) | Patiromer | SZC (Modern) |
|---|---|---|---|
| Onset Speed | Slow | Moderate (4-8 hrs) | Fast (<1 hr) |
| Sodium Load | High | Low/Neutral | Moderate |
| Main Risk | Colonic Necrosis | Hypomagnesemia | Edema (fluid buildup) |
| Cost | Budget-friendly | Expensive | Expensive |
Putting it All Together: A Management Roadmap
Managing hyperkalemia is a team effort involving your nephrologist, a renal dietitian, and a pharmacist. The goal is to keep your serum potassium in the "sweet spot" of 4.0 to 4.5 mmol/L. If your levels start creeping up, the process usually follows this path: first, a 48-hour window for dietary counseling, then optimizing your medication doses within a week, and finally starting a binder if levels don't budge after two weeks.
Be careful with timing. Some binders can interfere with other meds. For instance, Patiromer can reduce the absorption of levothyroxine by about 23%. If you're taking thyroid medication, make sure there is a 3-hour gap between the two. These small details are the difference between a treatment that works and one that fails.
What are the first signs of high potassium?
Hyperkalemia is often "silent" until it's dangerous. However, some people notice muscle weakness, a tingling sensation in the hands or feet, or heart palpitations. Because these are vague, regular blood tests are the only reliable way to catch it early.
Can I eat any fruit if I have CKD?
Yes, but you have to be selective. Swap high-potassium fruits like bananas and oranges for low-potassium options like apples, berries, and grapes. Portion control is key-even low-potassium foods can add up if you eat too many.
Why do my doctors insist on RAASi if it raises potassium?
RAASi medications significantly reduce the risk of heart failure and slow down kidney decline. The benefit of keeping your heart and kidneys stable usually outweighs the risk of high potassium, which is why doctors use binders to manage the potassium instead of just stopping the medication.
Is SZC better than Patiromer?
It depends on your needs. SZC works much faster, making it the drug of choice for acute spikes. Patiromer is often preferred for chronic, long-term use because it has a more neutral sodium profile, which is better for those with severe fluid retention.
What happens if I ignore a potassium level of 5.5 mmol/L?
A level of 5.5 is the threshold where medical intervention is strongly recommended. If ignored, levels can climb to 6.0 or higher, where the risk of sudden cardiac arrest or lethal arrhythmias increases dramatically.






12 Comments
Sam Hayes
April 5, 2026 at 15:29
just a heads up that leaching potatoes by soaking them in water for a few hours can actually pull out some of that potassium so you can still have them occasionally
simran kaur
April 5, 2026 at 21:18
of course they want us on these binders that cost a fortune while they push the RAASi meds that cause the problem in the first place
it is all a cycle designed by big pharma to keep you dependent on multiple prescriptions for a "problem" they created
Joseph Rutakangwa
April 7, 2026 at 10:52
good tips here
Will Baker
April 8, 2026 at 11:03
imagine actually believing that a smartphone app is the solution to a systemic biological failure
how quaint that we think barcodes can save us from heart failure
Mark Zhang
April 10, 2026 at 03:32
It's really tough balancing these dietary needs with the emotional toll of chronic illness. Just remember that you aren't alone in this struggle, and taking it one day at a time is a huge victory in itself. Keep pushing forward!
Jenna Carpenter
April 11, 2026 at 21:17
you guys really need to look at your inner energy flow becaus medications are just band-aids for a spiritallly blocked kidney. if you just align your vibrations you wont need these expensiv binders lol
Joey Petelle
April 12, 2026 at 02:51
the sheer audacity of suggesting berries as a replacement for a proper meal is just peak medical mediocrity
this is why the glorious American healthcare system is a joke, we're basically treating patients like toddlers with a snack list
Aysha Hind
April 12, 2026 at 15:42
The pharmaceutical industry is laughing all the way to the bank with these "modern solutions" like SZC and Patiromer
They create a chemical imbalance with one drug and then sell you the cure for a premium price it is a classic shell game to drain your wallet while you're too sick to notice the scam
sophia alex
April 14, 2026 at 12:01
Um, excuse me? The cost is irrelevant when the quality of care in this country is what truly matters 🙄 Only a true patriot understands that our medical innovation is lightyears ahead of the rest of the world! ✨
Vicki Marinker
April 15, 2026 at 05:07
The prose is marginally acceptable, but the obsession with "budgets" is utterly tedious. One wonders why we must quantify every morsel of food as if we are accounting for a failing corporation rather than simply existing.
Dee McDonald
April 15, 2026 at 07:01
LET'S GET AFTER IT! Managing CKD is a battle but you can win it with discipline and the right team! I want to see everyone tracking their levels and smashing those goals! Get those apple snacks in and keep your heart strong! YOU GOT THIS!
Hope Azzaratta-Rubyhawk
April 16, 2026 at 08:50
It is absolutely imperative that every patient adheres to these guidelines with the utmost rigor. Failure to monitor potassium is not merely a mistake, it is an act of negligence toward one's own survival. Be disciplined and stay alive!