Cell Lymphoma: Signs, Types, and What to Do
Notice a lump in your neck or armpit and worry it might be cancer? Cell lymphoma covers a group of cancers that start in immune cells. Some are fast, some move slowly. Knowing the common signs and what tests to ask for makes a big difference.
What cell lymphoma looks like
The most common early sign is painless swelling of lymph nodes—neck, armpit, or groin. Other frequent clues: unexplained fevers, drenching night sweats, sudden weight loss, long-lasting fatigue, and itchiness. Skin changes can be the first sign in cutaneous T‑cell lymphoma—think persistent rashes, patches, or plaques that don’t respond to usual creams.
Symptoms vary by subtype. B‑cell lymphomas (like diffuse large B‑cell or follicular) often cause lumping of nodes and systemic symptoms. T‑cell lymphomas can affect skin, blood, or internal organs and may behave differently. If symptoms last more than a few weeks, get checked.
How doctors confirm it
Diagnosis starts with a physical exam and blood tests. Imaging (CT or PET scans) shows where the disease is. The only way to know for sure is a biopsy—usually removing a whole lymph node or doing a core needle biopsy. Pathology labs use special stains and tests (immunophenotyping, flow cytometry) to tell B‑cell from T‑cell and identify markers that guide treatment.
Sometimes doctors need a bone marrow biopsy to check if the disease spread there. Ask your team to explain the exact subtype and stage—those details shape your options and outlook.
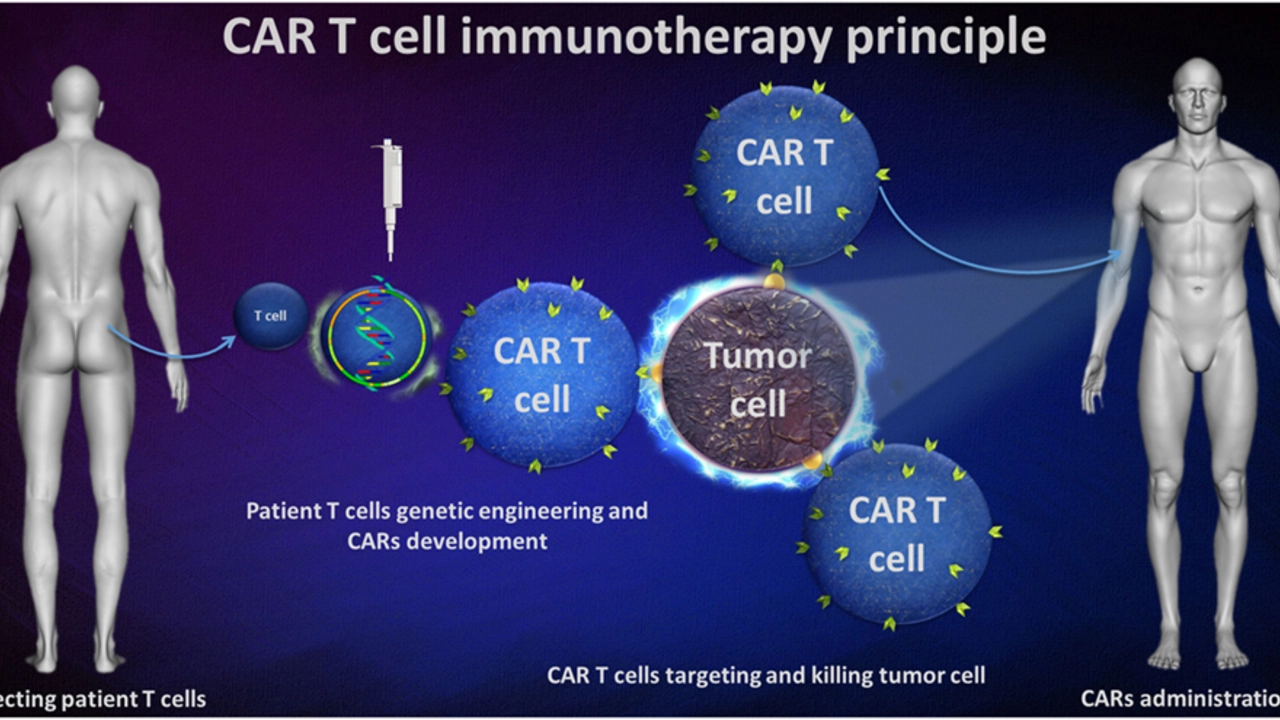
Treatment choices depend on subtype, stage, and your overall health. Standard options include chemotherapy, targeted drugs, monoclonal antibodies (like anti‑CD20 for many B‑cell types), radiation, and for some people stem cell transplant. Newer choices—CAR‑T cell therapy and other immunotherapies—are used for certain relapsed or aggressive cases. Cutaneous T‑cell lymphoma often responds to skin‑directed treatments such as topical meds, phototherapy, or systemic drugs when needed.
Side effects matter. Ask about expected short‑term effects (nausea, fatigue, low blood counts) and long‑term risks. Make a plan for infection prevention, managing fatigue, and nutrition—small steps help you stay stronger during therapy.
Practical tips: take someone to appointments, bring a list of your medicines, record questions, and ask for clear next steps after each visit. Consider a second opinion for major treatment decisions—especially if transplant or experimental therapies are on the table.
Want specifics for your case? Note the subtype name from your biopsy report and search for that exact term when looking up options. Patient groups, hospital cancer centers, and clinicaltrials.gov can point you to trials and specialists.
If you’ve found a lump, unexplained fevers, or persistent skin changes—don’t wait. See a doctor, get the right tests, and push for a biopsy if needed. Early clarity lets you choose the best treatment faster and protect your health.
The Importance of a Strong Support Network for Cell Lymphoma Patients
Living with cell lymphoma is a challenging journey requiring strong support networks for patients. These networks offer emotional, physical, and psychological aid that significantly contribute to the patient's well-being and recovery. Loved ones, friends, healthcare professionals, and support groups play vital roles in offering comfort, understanding, and practical assistance. They provide a sense of belonging, reduce feelings of isolation, and help patients cope with the disease's physical and emotional toll. In essence, a robust support network is a lifeline for cell lymphoma patients.
Read More