Cause — What Triggers Diseases, Drug Reactions & Medication Side Effects
Sometimes the reason you feel worse isn’t the disease — it’s the cause behind it. A single trigger, like smoking or a food interaction, can change how a medication works or how a condition progresses. You don’t need a medical degree to spot common causes. You need a checklist and a few smart habits.
Common types of causes you’ll see
There are a few repeat offenders. First: lifestyle causes. Smoking is the main driver of emphysema and COPD — that’s the core point in our emphysema guide. Diet and alcohol also push many conditions forward. Second: drug-related causes. Some foods and supplements change drug levels — grapefruit and other citrus fruits famously do this, and our citrus interactions piece explains which meds are affected. Third: mistakes and risky sources. Buying meds from unverified online sellers can introduce unsafe products or wrong dosages — we cover safe buying tips in articles like how to buy Zyvox online and guides on buying peptides and affordable antibiotics.
Genetics and infections are other big categories, but they’re often paired with something modifiable — lifestyle, environment, or medication errors. Identifying which category a problem fits into makes fixing it much simpler.
Medication-related causes: quick examples that matter
Drugs have specific vulnerabilities. Diuretics like Lasix can drop potassium and cause dizziness or muscle cramps if you don’t monitor electrolytes. Blood pressure meds such as Cozaar (losartan) can affect kidney function in some situations. Antibiotics like Bactrim and stronger drugs like Zyvox can interact badly with other prescriptions or supplements. Even over-the-counter inhalers and supplements can trigger real harm if mixed with the wrong prescription — the Primatene Mist and supplement discussions show why reading labels matters.
Also watch for counterfeit or poorly labeled products when buying online. Fake or substandard meds are a direct cause of treatment failure and harm. Our buying guides show what to check: pharmacy credentials, clear contact info, and realistic pricing.
Want to figure out a cause fast? Start with a short list: what you ate, what you took (prescription and nonprescription), recent infections, and any new habits. That simple list solves a surprising number of mysteries.
Practical steps to reduce risk: keep a current medicine list, use an online interaction checker or ask your pharmacist, read product labels, avoid risky online vendors, and schedule a quick check with your clinician if symptoms change after starting a new drug. If a cause looks unclear or serious, get medical advice rather than guessing.
We’ve got focused reads on many of these causes — from citrus interactions to Lasix, from emphysema causes to safe online buying. Browse those articles for specifics tied to your situation and use the practical tips there to lower your risk and make smarter choices about treatment and prevention.
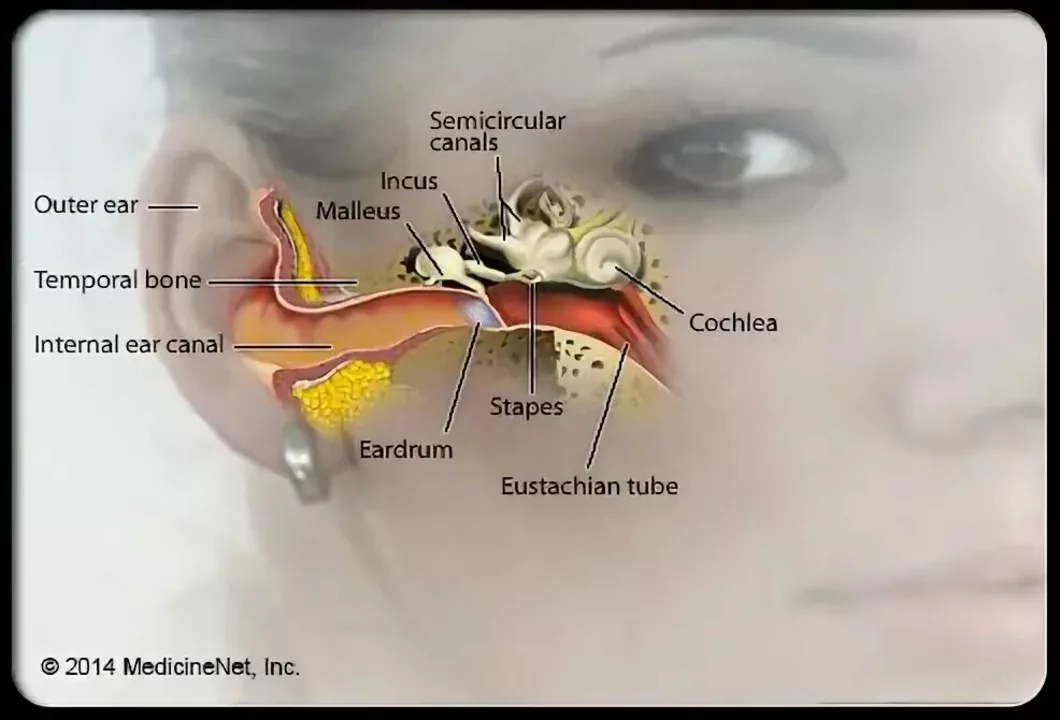
Atenolol and Tinnitus: Can It Cause Ringing in the Ears?
I recently came across some information on Atenolol and tinnitus, which got me thinking - can this medication cause ringing in the ears? From my research, it seems that Atenolol, a beta-blocker used to treat high blood pressure and other heart conditions, has been linked to tinnitus in some cases. Although it's not a common side effect, some people have reported experiencing ringing in their ears after taking Atenolol. If you're on this medication and notice any changes in your hearing, it's essential to consult your doctor. They can help determine if Atenolol is the cause and recommend alternative treatments if necessary.
Read More




